Free National Healthcare In Jamaica – Promise Or Peril?
It is extremely expensive, with estimates as high as $US15000, to provide the currently recommended medications for the care of one HIV positive patient each year in Jamaica.
HIV, in a large number of cases, is a preventable lifestyle disease. Assuming 1.5% of the population is HIV positive the total projected yearly cost to provide optimal care for uncomplicated patients combined is about US$675 M. Since the prevalence of HIV is stable this is a recurring yearly expenditure.
The cost to dialyse one ESRD {End Stage Renal Disease} (“Kidney”) patient three times each week and thus 156 times each year is significant. Early management of Hypertension and Diabetes Mellitus as well as Obesity prevention can reduce the burden of ESRD.
In every society the economic costs attributed to Smoking associated diseases including Lung and other cancers, Asthma and Chronic Obstructive Pulmonary Disease (COPD/ Bronchitis) is staggering.
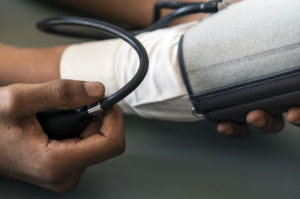
Lifestyle diseases including Hypertension (“Blood pressure”), Diabetes Mellitus (“Sugar”), Hyperlipidemia (Cholesterol”), Obesity (“Overweight”) and Osteoarthritis (“Arthritis”) each exact their enormous, unique, and cumulative economic toll.
Wisely, the Health Minister, Dr Christopher Tufton, has consistently attempted to engage the Jamaican population around positive behaviours to minimise the number and impact of these lifestyle diseases. Jamaica moves is one such program. More recently attention has been directed at reducing sugar intake with obesity and diabetes reduction clear targets.
Dr. Fenton Ferguson, the former PNP Health Minister, boldly introduced legislative changes to reduce cigarette smoking and the multiple co-morbidities associated with it’s negative and unhealthy practice. The decisions and actions of these most recent Heath Minsters are forward thinking and deserving of accolades. Their actions demonstrate an understanding of the economic and other challenges all societies face regarding the delivery of healthcare to their populace. In most societies including Britain, the USA, and Canada the percentage of GPD dedicated to satisfying health care cost has been increasing in a worrisome way.
Jamaica, not surprisingly, is facing this same challenge regarding the delivery of high quality, efficient, and cost effective healthcare.
Does Jamaica have the capacity to indefinitely offer free healthcare to all its citizens? Many attribute the problems with inefficiency, poor quality care, hostile and unprofessional work environment, caregiver fatigue and burnout to this free care for all approach. The healthcare budget is limited, a reflection of government budgetary constraints.
Many conclude the absence of patient accountability, responsible behaviour and the impact of the “freeness mentality” contribute immeasurably to the multiple healthcare delivery challenges. In the USA a major family health emergency not infrequently can result in bankruptcy, thus wrecking, economically, ones future! Do many Jamaicans get exposed to this oppressive financial burden when health emergencies arise?
The Jamaica healthcare system usually lurches from one crisis to another. The highly publicised Cornwall Regional Hospital closure due to years of neglect and decay immediately comes to mind. No sustained, ongoing effective preventative maintenance was in place. Note the dead babies saga at the University of the West Indies (UWI) Hospital. Concern was raised at the time about the absence of preventative upgrades in needed equipment. Delivery of care at the Kingston Public Hospital (KPH) was significantly impacted for several months due to an elevator failure. Standard, acceptable preventative maintenance could have minimised the down time of this essential equipment.
Diaspora engagement is now being negatively impacted by the perception that hard earned well meaning contributions are wasted. Donated essential equipment languishes indefinitely on the wharf waiting to be cleared. Concerns abound that smaller machines and medical devices disappear from public healthcare facilities to the offices of private practitioners enriching them instead of serving the population for whom the donation was made. But most alarming is the perception there are no well laid out strategic plans to facilitate steady improvement in overall healthcare delivery. The conclusion is, the leadership in society because of political partisanship and cronyism is, wedded to these outdated failed practices. Donors now are closing their check books until satisfied these pressing, prudent concerns are addressed. Past, but recurring, fits and starts have unfortunately resulted in mounting giver fatigue.
So immense economic pressure is mounting on the healthcare budget as the sector grapples with developing and deploying useful mechanisms for optimal delivery of evidenced based, high quality care. Will the system continue to depend on sporadic contributions – like the planned $4M third year UWI medical students smoker contribution – to band-aid real major healthcare system challenges? Will all patients be required to contribute at some pre-determined level irrespective of financial means?
Can insured patients be identified and required to pay their honest portion? Should patients attending public healthcare facilities be given staggered appointments? Six patients for eight o’clock, six more for nine o’clock and so on. Rather than all one hundred being given the same eight o’clock appointment. Employers can be required to share insurance coverage information of employees with all government sponsored pharmacies. Before prescriptions are filled the insured data base can be interrogated and the appropriate cost to the insured patient applied. Novel solutions are difficult but not impossible.
Kicking the proverbial can down the road will result in no different fate than that which overcame the Cornwall Regional Hospital. Meanwhile the ones responsible for blindly overseeing the demise of the system will, in hindsight, immaculately acquire perfect twenty-twenty vision when no longer in charge and the system predictably crashed. These, now astute, none performers will even blindly, and opaquely offer magical prescriptions to resolve long standing healthcare dilemmas they had haplessly, previously mismanaged.
Welcome to Jamaica where reality and fiction seem. inseparable!
Until genuine reality surfaces, many in the diaspora eagerly await the opportunity to make significant and meaningful contributions to the beautiful Jamaica, ‘land we love’.
By Guest author: Leon Wright.
Download The Jamaican Blogs™ App for your Android device: HERE
Remember to share this article on Facebook and other Social Media Platforms. To submit your own articles or to advertise with us please send us an EMAIL at: [email protected]



